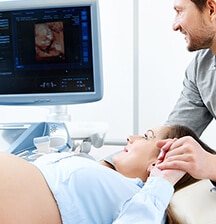
For many women, having a glass of wine with a meal or to celebrate an event is a common occurrence. But what happens when they fall pregnant? Do expectant mums really need to give up their favourite tipple, or can they still have that odd glass of wine? Christine Rogan explains.
A baby on the way is a beautiful thing. But let’s face it, women who happen to be pregnant are subjected to a lot of advice; some of it irksome. Having children certainly requires significant adjustment to one’s priorities and for women that starts at conception. On the list is giving up alcohol. For women used to socialising with alcohol this can seem like a sacrifice rather than something beneficial.
The majority of women understand that alcohol should be avoided during pregnancy and stop drinking when they know they are pregnant, which is good news, but sadly, not everyone does. The trouble is that alcohol is almost universally available and drinking has become so normalised that it can be difficult to imagine a social occasion without it. Many women may not have been advised to stop or believe that drinking while pregnant isn’t harmful. Around a quarter of New Zealand women report drinking knowing they are pregnant. Does it matter and is it a risk worth taking? Alcohol is a neuro-toxin with no known safe level of consumption – for adults, let alone children. Socially, we have learned to use alcohol to fit in, relieve stress, overcome boredom, drown sorrows, celebrate success – and that adds up to a lot of alcohol before anyone suggests there might be a problem. Even more confusing, alcohol is a drug that is categorised as a food. With such a social backdrop, it is easy to gloss over the harmful effect, or to think this is a problem for others but not ourselves. However at a basic level, we are all biologically susceptible to chemicals and the womb affords us no protection before we are born. Alcohol is a teratogen, a term used to describe a substance that can reach the baby through the placenta and alter normal development. Alcohol exposure can cause physical birth defects, neurological damage, growth retardation or even death, depending on dose and timing. Heavy alcohol use or ‘binge’ drinking (4 or more units of alcohol per occasion for women) is more likely to cause harm. The more often such drinking occurs, the more likelihood of damage. Babies exposed to alcohol through their mother’s drinking may be born with Fetal Alcohol Spectrum Disorder (FASD). FASD is a range of significant learning and behaviouraproblems, some of which are obvious from the start and others that don’t stand out until the child reaches school-age and starts to fall behind. These are permanent brain deficits caused by alcohol and are not something the child will outgrow. They are often misunderstood or misdiagnosed.
Individuals with FASD are more likely to experience adverse outcomes than the general population, particularly in adolescence and adulthood when there has been insufficient or inappropriate accommodation of their disability. Referred to as secondary disabilities, these adverse outcomes include mental health problems, addictions, education failure, committing or being a victim of crime and having difficulties maintaining employment. They too are preventable and worthy of investment.
So avoiding binge-drinking, to minimise the chance of a child being born affected by alcohol (and potentially FASD), is important, and better for mum’s health too. But what about light drinking? Is there nothing wrong with a glass or two now and again, as claimed in some media headlines? While such claims may present some women with reassuring news, there is much these studies, flouted by the media, don’t tell us. The methods these studies employ would not be sensitive enough to pick up subtle changes in brain function due to the effects of alcohol at low levels of prenatal exposure, but that does not equate with safety. Other types of studies detect brain deficits at very low levels of consumption. Clearly, science has yet to determine whether a safe amount exists, or even if this is possible. However, we do know that alcohol can reach the baby through the placenta – so should pregnant mothers really take the risk?
Health authorities around the world, and the New Zealand Ministry of Health, are very clear that there is a risk to health and they advise no drinking during pregnancy or when planning to be pregnant. Unfortunately, there is very little public awareness to strengthen this message, no government warning on the bottles or where alcohol is sold, and little training of frontline health professionals to counter misinformation. These factors all need to be working together for pregnant women to be well-informed about the risks of alcohol to their unborn child.
It is worth ditching the booze for the sake of the next generation. Our babies will thank us in the long run!
For concerns about alcohol-related problems, phone the Alcohol Drug Helpline: 0800 787 79
Christine Rogan is a Health Promotion Advisor for the Alcohol Healthwatch Trust based in Auckland. Christine draws on over 17 years of experience and evidence in the FASD field and 26 years as a mother